

Many EMS protocols recommend administration of lidocaine through intraosseous access before flushing to decrease the associated pain, but how effective is this? Literature supporting the practice is very sparse.
Thirty-six patients with GCS above 8 rated pain associated with IO insertion at 3.8, and pain from fluid infusion averaged 5 on a modified visual analog scale (1-10). Eleven of the patients who received lidocaine reported reduced pain. The IO insertion location wasn’t specifically mentioned, but based on common practice when the study was published, it was most likely proximal tibia. Davidoff 2005
Among 32 combat casualties treated by the UK in Afghanistan, all responsive patients reported pain with IO infusion. Three stated that IO infusion pain was worse than their traumatic injuries. Cooper 2007
In an abstract, never fully published, 10 adult volunteers, with proximal humerus IO access, received various doses of IO lidocaine followed by a “hard flush” of saline and additional lidocaine. On a visual analog scale, mean insertion pain was 3.9 +/- 1.5. After 20 mg IO lidocaine, the highest score was 2.0 +/- 1.2 at IO fluid administration pressures of 300 mmHg. Philbeck 2009
The most detailed studies to look at the issue of IO associated pain were manufacturer associated and therefore at risk of bias. Two non-randomized studies involving 10 volunteers each underwent IO insertion at either the left / right proximal tibial or proximal humerus.
Mean insertion pain at the left tibia was 4.4 +/- 2.6, right tibia 3.6 +/- 2.3, and 3.0 +/- 1.5 for proximal humerus.
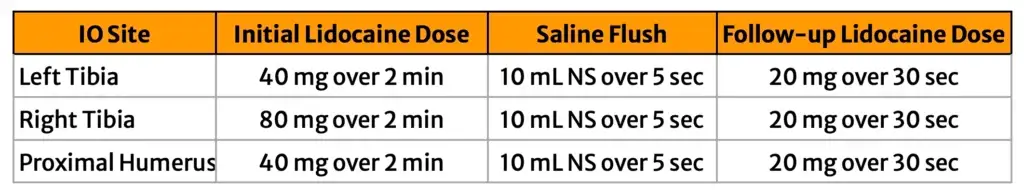
Left Tibial - 40 mg lidocaine over two minutes, flushed with 10 ml saline over five seconds, and finally an additional 20 mg lidocaine over thirty seconds.
Volunteers undergoing tibial insertion received different IO lidocaine dosing based on IO location.
Right Tibial - 80 mg lidocaine over two minutes, flushed with 10 ml saline over five seconds, and finally an additional 20 mg lidocaine over thirty seconds.
Proximal humerus - 40 mg lidocaine over two minutes, flushed with 10 ml saline over five seconds, and finally an additional 20 mg lidocaine over thirty seconds.
Pain at the left tibia was 6.8 +/- 2.9, right tibia 7.9 +/- 2.8, and 4.6 +/- 2.9 for proximal humerus. These measurements appear to follow the first lidocaine bolus. The authors concluded that 40 mg and 80 mg lidocaine doses provided equivalent tibial pain control.
Finally, in a study including 22 prehospital patients felt to be “conscious and alert,” who received IO access, none described the needle insertion as painful. However, despite 12 patients receiving 20 to 40 mg lidocaine before fluid administration through the IO line, 18 reported pain with IO use. One with multiple injuries had so much intramedullary pain from the IO fluid administration it had to be stopped. Schalk 2011
Other authors acknowledge it is unclear if lidocaine administration after IO access decreases pain significantly or not. Reasonably, they note for conscious patients it takes little time, may help, and is unlikely to cause harm.
1 – IO flushing is uniformly painful
2 – Humeral IO sites may have less associated pain than tibial sites.
3 – Flushing causes more pain than initial insertion.
4 – 40 mg IO lidocaine over two minutes, followed by rapid normal saline flush, then another 20 mg IO lidocaine over 30 seconds showed best pain control at the both the humeral and tibial sites.
5 – When additional lidocaine is needed it occurs at around 20 to 60 minutes post infusion initiation.
Clinical Note: If IO lidocaine is to be used, it must be preservative free, which is typical for the lidocaine in code carts, but not lidocaine used for wound anesthesia.
Davidoff J, Fowler R, Gordon D, Klein G, Kovar J, Lozano M, Potkya J, Racht E, Saussy J, Swanson E, Yamada R, Miller L. Clinical evaluation of a novel intraosseous device for adults: prospective, 250-patient, multi-center trial. JEMS. 2005 Oct;30(10):suppl 20-23. PMID: 16382512.
Cooper BR, Mahoney PF, Hodgetts TJ, Mellor A. Intra-osseous access (EZ-IO) for resuscitation: UK military combat experience. J R Army Med Corps. 2007 Dec;153(4):314-6. PMID: 18619171.
Philbeck TE, Miller LJ, Montez D, Puga T. Research Abstract, Annals of Emed Med 2009.
Philbeck TE, Miller LJ, Montez D, Puga T. Hurts so good. Easing IO pain and pressure. JEMS. 2010 Sep;35(9):58-62, 65-6, 68; quiz 69. doi: 10.1016/S0197-2510(10)70232-1. PMID: 20868946.
Schalk R, Schweigkofler U, Lotz G, Zacharowski K, Latasch L, Byhahn C. Efficacy of the EZ-IO needle driver for out-of-hospital intraosseous access–a preliminary, observational, multicenter study. Scand J Trauma Resusc Emerg Med. 2011 Oct 26;19:65. doi: 10.1186/1757-7241-19-65. PMID: 22029625; PMCID: PMC3212886.